Campylobacteriosis is the most common notifiable infectious intestinal disease in New Zealand. Infection causes diarrhoea and vomiting, and in a small number of cases, a long term illness or even death.
ESR and Massey University in association with certain North Island district health boards, conducted the SACNZS on behalf of the Ministry of Primary Industries. The study investigated campylobacteriosis cases in Auckland, Manawatu, and Whanganui over the course of a year (2018-2019) to determine the different contributors to the disease, help manage the risks associated with campylobacteriosis, and inform policies for prevention and control.
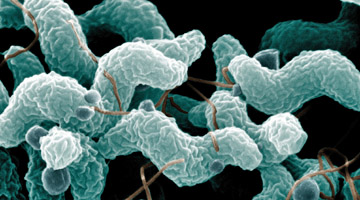
Campylobacter jejuni bacteria
There are many possible sources of and ways to become infected with Campylobacter. The study assessed the following three main categories that are associated with infection:
- Animal sources: poultry, cattle, sheep, pets, wildlife
- Exposure pathways: environment/water, food chain, direct contact
- Risk factors: drinking water sourced from rainwater/roof tank, swimming in a river or lake, eating BBQ poultry, drinking raw milk, working in a poultry abattoir, rearing a pet calf

Rearing a calf is a risk factor for contracting campylobacteriosis
The study combined interviews with people infected with Campylobacter and laboratory methods to identify the sequence of DNA in bacteria isolated from infected people and livestock. These methods allowed researchers to assess where the Campylobacter infection was likely to have originated.
Several significant risk factors for contracting campylobacteriosis were identified. They were:
- Eating undercooked poultry, and eating poultry outside the home
- Living and/or working on a farm and direct animal contact, particularly for cattle-associated cases.
- Drinking raw milk, specifically for urban cases that were cattle-associated.
- Rainwater/roof tank as a water source, either in the home or elsewhere
- Using prescribed proton pump inhibitors as a medication which reduces the acidity of the stomach, a barrier to infection.
- Close contact with another person with gastrointestinal symptoms.
Taking into account both the source of infection and specific risk factors for human campylobacteriosis, the study demonstrated that poultry meat remains the dominant pathway for exposure and infection in New Zealand, especially for urban dwellers. Poultry was likely to have been the source of around 90% of illnesses in urban-dwelling people. The study highlighted the importance of managing risks within the poultry industry to reduce Campylobacter infection in New Zealand.
To find out more about how MPI works to reduce the number of cases of campylobacteriosis related to food, read their Campylobacter risk management strategy:
Campylobacter risk management | NZ Government (mpi.govt.nz)(external link)
